Interview: “Exponential rise in mucormycosis in India is alarming; not seen this anywhere in the world”
Shrikant Ambalkar, the UK-based consultant in clinical microbiology and infection specialist, spoke with Gaon Connection about the reasons behind the rise of ‘black fungus’ infection cases in India, and what can be done to prevent mucormycosis. Watch the detailed interview.

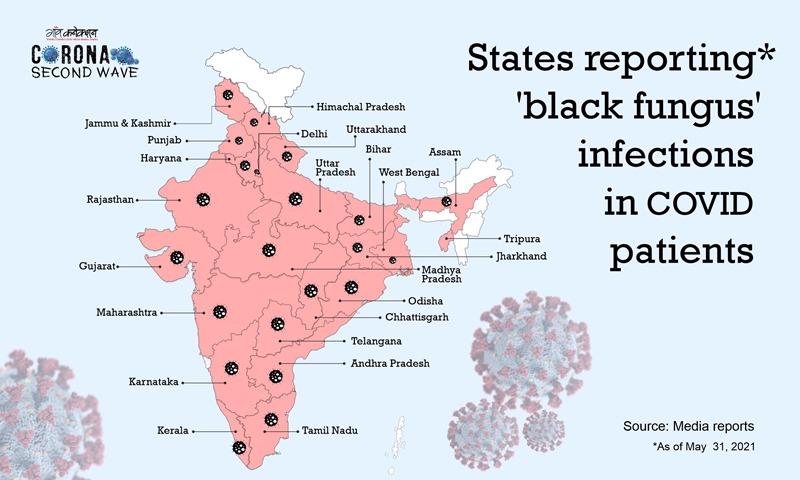
While dealing with the second wave of the COVID19 pandemic, India is tackling another epidemic — mucormycosis — which is also commonly known as ‘black fungus’ infection.
Recently on May 24, the Union Health Minister Harsh Vardhan informed that, of the 5,424 cases of Mucormycosis, nearly 84 per cent cases have a history of COVID19 infection, while 16 per cent are amongst non-COVID patients. Diabetes was present in 55 per cent of the patients.
Maharashtra and Gujarat are the worst affected states. Meanwhile, on May 19, the Union health ministry asked states and union territories (UTs) to declare black fungus a notifiable disease under the Epidemic Disease Act, 1897.
Apart from the black fungus infection cases, patients suffering from white, yellow, cream and a new fungal infection called aspergillosis have been reported in India.
To understand the rising fungal infections, their symptoms, treatment and prevention, Gaon Connection spoke with Shrikant Ambalkar, a consultant in Clinical Microbiology and Infection specialist, who is based in the United Kingdom. Ambalkar is a key member of the COVID-19 management group in the Sherwood Forest Hospitals NHS Trust.
Here are the excerpts from the video interview:
What about the sudden rise in fungal infections in India?
We have seen an increased number of [mucormycosis] cases in COVID patients over the last eighteen months. Few cases were reported in China last year. There is a definite correlation between invasive fungal infections and COVID19.
We have not had many mucormycosis cases in my hospital. We have seen many other fungal infections such as aspergillosis. But in India we are seeing an exponential rise. This is really alarming. We have not seen this anywhere in the world.
What are the risk factors? Who are the vulnerable groups?
The most common fungus is called a mold. Aspergillosis and mucormycosis are present in the environment everywhere. People with normal immune systems do not get these infections. Only those with less immune system, such as patients of cancer and HIV — where there is immunity is suppressed.
Another risk factor is indiscriminate use of steroids. It suppresses your immune system which makes one susceptible for infections.
Although steroids have been found beneficial in the treatment of COVID 19 patients. However, not with those with mild infections.
My perception is steroids have been extensively used in India for treatment of COVID patients, even for mild infections that probably has caused sudden rise in mucormycosis cases.
Diabetes is another risk factor. Uncontrolled diabetes causes hyperglycemia. Fungal loves hyperglycemia, high glucose, immunosuppression and damage caused by the coronavirus.
Why are mucormycosis cases rising now?
COVID cases have been rising exponentially during the second wave. It is a proportional case in the rise of mucormycosis.
Steroids have been used for a long time and for so many other reasons. However, it is wrong to say this is happening now. As per a paper released by experts in Jaipur [Rajasthan], they have reported a significant number of mucormycosis cases before the second wave. There are many patients who have got infected with mucormycosis even when they were not put on steroids or were not diabetic. Studies need to be conducted on this.
Is there a role of zinc and antibiotics behind the outbreak?
Many hypotheses are floating around on social media. Whether zinc or industrial oxygen or antibiotics are responsible. I suggest at this moment of time we need to do thorough study on this. Zinc promotes the growth of mucor. Unless we do a scientific investigation then only we will know the cause.
The second wave has also affected the rural population of the country. Are villages at risk of the rising fungal infections too?
There is nothing distinctive that makes village population more susceptible for mucormycosis. There are the same risk factors such as diabetes and increased use of steroids, and the virus itself. They can cause mucormycosis in that group of patients as well.
The only problem with rural India is the lack of facilities to monitor patients. Moreover, post-COVID management is not possible in the rural setting. It is difficult to monitor their blood sugar levels.
What can we do to prevent this infection?
Controlling the risk factor is important. We should not be using steroids unnecessarily. We need to monitor high risk patients regularly. We also need to inform the patient that these are the things you should look for and then seek medical help. This is how we can control it.

