How did India’s most populous state Uttar Pradesh lead the COVID-19 battle?
Aggressive testing, COVID care hospitals, surveillance and isolation, ration kits for migrant workers, and record vaccination of healthcare workers are a few measures adopted by the state government. How do experts rate the response?


Yogi Adityanath, chief minister of UP, while inaugurating a dedicated 400-bed government hospital for COVID-19 patients in Noida, last year in August. Photo: @CMOfficeUP/twitter
Lucknow, Uttar Pradesh
On March 4 last year, Uttar Pradesh recorded its first case of COVID-19 in Ghaziabad. It’s been a long, arduous journey since then for India’s most populous state with a population of over 240 million — nearly 10 times that of Australia. As of today, March 6, the total COVID-19 cases in Uttar Pradesh stands at 0.604 million, of which 98 per cent have recovered. The state, which recorded 6,777 cases a day last September — the highest spike in COVID-19 cases a day — reported about 119 cases today. Over 8,700 people have lost their lives to the virus in the state. The death rate due to COVID-19 in the state is 1.3 while the recovery rate has shot up to near 90 per cent.
To manage the crisis here, a multi-pronged strategy was adopted, claims the state government. Boosting overall health infrastructure, aggressive testing, contact tracing, surveillance and isolation, adhering to public health guidance and vaccination were a few of the measures adopted.
As of now, Uttar Pradesh has a total of 674 COVID-19 hospitals — 571 level one (to treat very mild, mild and suspected cases), 77 level two (for clinically moderate-level serious patients) and 26 level three (to provide comprehensive care to severe and critical patients) COVID hospitals. The total availability of beds in these hospitals is 157,000. This number was near zero in March last year. Also, as per the state government, all 75 districts in the state have at least one level two COVID hospital, with provision for ICU beds.
“Our fight with COVID is still going on. The results are good too. We see many villagers come for COVID tests. They cooperate with us. But I think the ‘micro interiors’ [infrastructure quality] of village centres should be improved,” Alam Husain, an AYUSH doctor from Sant Kabir Nagar district, Uttar Pradesh, told Gaon Connection. He works in a community health centre that was converted into a level one COVID centre.
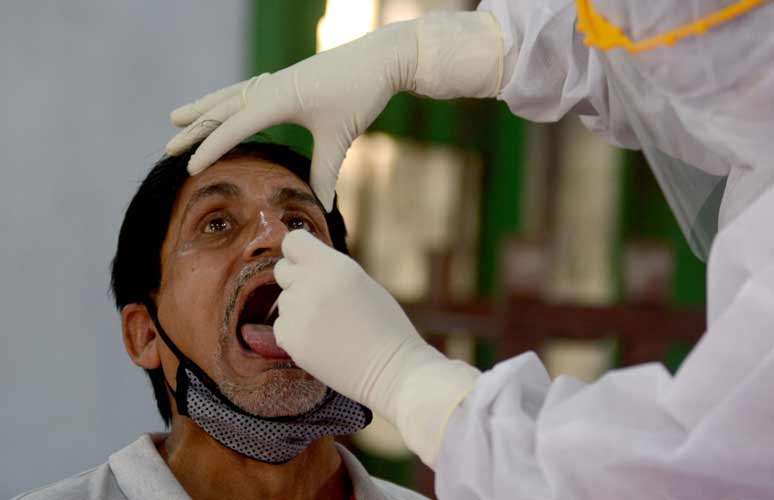
Increased testing
Uttar Pradesh is now testing above 0.15 million samples a day for the COVID-19 virus. Initially, the state did not have sufficient testing facilities. Last year, on March 22, when the 14-hour Janata curfew was announced, the state had only one testing lab and the testing capacity was just 60 samples a day. This has now gone up to 234 labs, including 131 government labs, claims the state government.
But is that enough?
“Going by the large population of the state, the number of daily tests conducted is not enough. Testing needs to be accelerated,” Sunita Singh, Lucknow-based member of the Jan Swasthya Abhiyan, a non-profit working in public health, told Gaon Connection.
Singh, who is working at the village level, also informed that many villagers complain that whenever they visit a health facility for regular checkups, they have to undergo a COVID-19 test. This, when those coming in from other cities have not undergone any tests. “There is no tracking system for people coming from cities such as Pune, Mumbai, Delhi or other COVID hotspots. They could be carriers. We need to observe whom we are testing, and who needs our service,” she said.

Meanwhile, people who have recovered from the disease seem satisfied with state’s response. Take the case of 29-year-old Abhishek Shukla from Prayagraj, who tested positive for the virus on October 2 last year, and was asked to isolate at home for 14 days. He was also given medicine free of cost for 10 days. “The facilities provided in the COVID care centre were satisfactory. The staff was very friendly. Apart from counselling us about social distancing, they also took care that we do not get too worried about the virus,” Shukla told Gaon Connection.
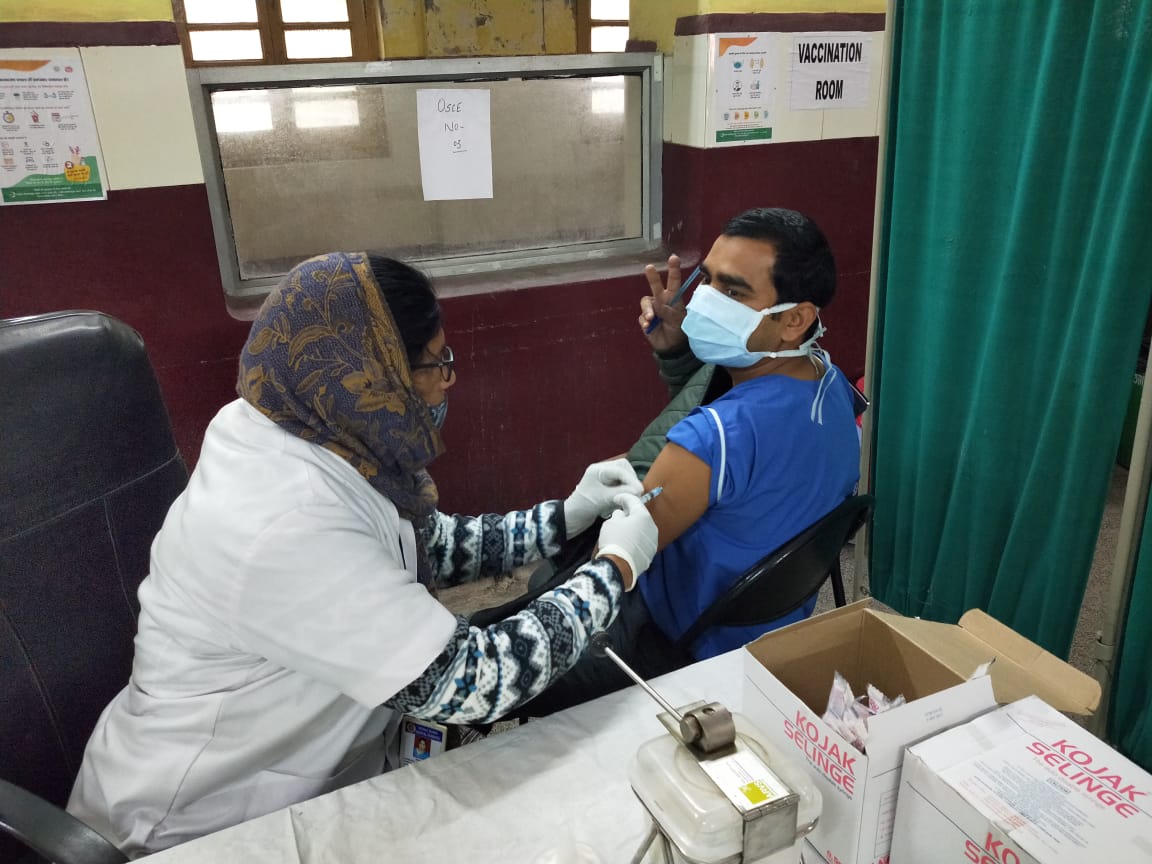
The Uttar Pradesh government also claims that it has carried out the most number of COVID-19 vaccinations — more than 0.643 million health and frontline workers have been vaccinated.
Integrated approach
On July 18 last year, the UP government set up an Integrated Control and Command Centre (ICCC) for monitoring of COVID-19 management. It ensured contact tracing, home visits by the health team for patients in home isolation and testing of all eligible persons. Besides, a continuous dialogue with COVID patients was maintained through the CM [chief minister] helpline number, and all patients were called to know about their wellbeing and any issue faced at the hospital level.
Shukla confirmed this. “After I tested positive for COVID, a team was sent to my home. Every day, I would get a call from the department asking about my body temperature and general health,” he said. Although he tested negative after 10 days, Shukla experienced post-COVID-19 side effects such as weakness for three months.
Post-COVID-19 care centres
This is why patients and health experts believe there is a need to set up post-COVID care centres in the state. Apart from other post-recovery complications, “patients tend to experience mental trauma, as people discriminate against them and avoid social or physical contact with even those who have recovered. This is very common at the village level”, said Singh. “Counselling of people post-COVID is also needed, and we need post-COVID care units for that,” she added.
The state government claims that each district hospital in the state will get a post-COVID care unit for those who face complications such as breathlessness and those with mental health issues.
Also read: Ready and Waiting: How willing are the villagers in Uttar Pradesh to be vaccinated against COVID-19?

The role of frontline workers
During the pandemic, the Uttar Pradesh government initiated training for medical staff to sensitise them about COVID-19, prevention protocol, treatment flow chart and other logistics. The state also procured protective gear for healthcare and frontline workers. The department of micro, small and medium enterprises (MSME), Uttar Pradesh, now manufactures medical equipment such as thermometers, pulse oximeters and PPE [personal protective equipment] kits. These were earlier procured from outside the state.
However, healthcare staff claim a lot more needed to be done. “We got surgical masks and sanitisers only two times. We can only use such masks once. We have to buy masks on our own,” an ASHA [Accredited Social Health Activist] sangini in Lucknow told Gaon Connection.
“Many people lost their lives to the virus. Now, the situation is under control, and so are the arrangements. The state government claims it has done enough, but when services were needed the most, not much happened,” she rued.
Also read: In this battle against the novel coronavirus, ASHAs have donned the role of Corona Warriors

Managing the migrant workforce
One of the biggest challenges before the state government was managing the influx of migrant workers from other cities during the COVID-19 lockdown. As per the state government, around 4.5 million migrant workers returned home amid the pandemic. To ensure basic facilities such as food and water to this many people, the state set up community kitchens.
About 67.5 million food packets were distributed to them during the lockdown period, and those sent to quarantine at home were given kits with ration for 30 days, the government claims. Each kit included 10 kilogrammes (kg) each of rice and flour, two kg of arhar dal (pulses), five kg of potatoes, one litre oil, and 250 grams of spices, including coriander power, chilli powder and turmeric powder, besides salt and two kg of roasted gram.
Also read: Migrant Workers: The Indian government does not know their numbers, dead or alive
“It is important to understand how many migrant workers availed of these benefits. A majority definitely did not get them,” Santosh Punia, member, Aajeevika Bureau, a non-profit working to enhance the dignity and wellbeing of migrant workers, told Gaon Connection.
“Food from community kitchens was supplied to these workers in quarantine centres. But, most workers complained they were not getting food at quarantine centres, and that their families were bringing food for them. This claim of the state government is wrong,” said Punia, who is based in Udaipur, Rajasthan, but works with organisations in Uttar Pradesh.

Also Read: 64% migrant workers were quarantined in villages, 9 in 10 didn’t undergo COVID-19 testing
According to the state government, apart from the ration kit, every migrant worker sent home was given a sustenance allowance of Rs 1,000 to help tide through the initial uncertainty. In addition to this, about 5.3 million construction labourers, street vendors, carriage pullers and daily wagers in rural areas were given Rs 1,000 each through direct benefit transfer.
But, Punia challenges such claims. “The cash assistance was not given to all workers. It was only for the registered workforce. Secondly, thousand rupees is insufficient for these workers to help people relocate,” he said.

