Meet the man who made the Bijapur District Hospital in Chhattisgarh one of the best
In 2016, when Ayyaj Tamboli, a doctor, joined as the Bijapur district collector, he was disappointed to see the plight of the district hospital. This is what happened next ...


The year was 2016. Dr Ayyaj Tamboli, now the collector and district magistrate of Bastar, Chhattisgarh, had moved to the Bijapur district, about 500 kms from the state capital Raipur. He had just taken over as the district collector.
“One day, an Adivasi woman came to the district hospital at Bijapur with her three-day-old baby, who was critical. The Naxals were not letting her stay back at the hospital for the night. We told her the baby needed support, but she was adamant and said the Naxals had threatened to kill her if she did not return the same day. Surprisingly, she asked us to keep the baby and went back,” said Dr Tamboli.
He added: “She came back two days later. She visited the hospital, on and off, over the next for 6-7 days and finally took the baby with her. The point is, if there is so much pressure on this section of society, which is also very poor, we must strengthen our district hospitals.”
Dr Tamboli dedicated the next one year and transformed the district hospital at Bijapur. What makes the transformation incredible is that Bijapur is densely- forested and a Naxal hotbed.

Created in 2007, it is one of the newly-formed districts in Chhattisgarh. It borders Telangana and Maharashtra. Earlier, Adivasis here had to travel 160 km to Jagdalpur, the administrative headquarters of Bastar district, for even basic medical facilities or deliveries. The district hospital in Bijapur was in poor condition and grossly understaffed, and not many doctors were ready to risk their lives working there.
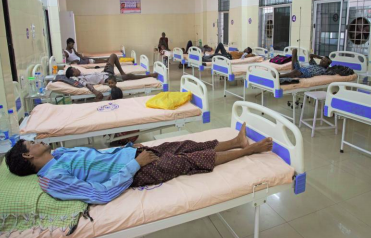
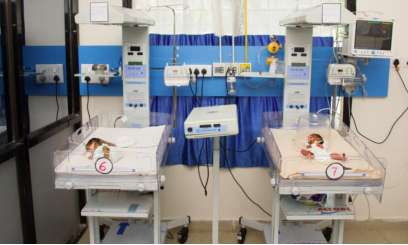
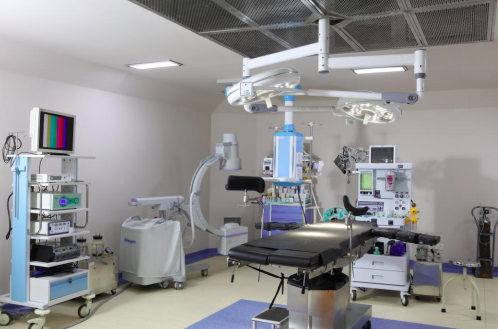
All that changed in 2016 when Tamboli — a doctor himself — took over as the Bijapur district collector. Within a year, he completely transformed the hospital. It became a 150-bed facility with brand new operation theatres and a new ICU. A blood bank and dedicated child health care units were also set up in record time.
In 2017-18, the hospital treated close to one lakh patients and handled 1,200 childbirth cases, of which 199 were caesarean. It also conducted about 2,000 other operations, including laparoscopic surgeries, for free. The hospital now has even advanced facilities like radiology and physiotherapy.
The transformation hasn’t gone unnoticed. The hospital won the second prize in the 2017-18 Kayakalp awards for health facilities instituted by the National Health Mission. This success story has led authorities to use the same blueprint to address many issues in the other Red Corridors — regions that experience Naxal activities — in the state.

Upgrading infrastructure, the first step
“We started this experiment in June 2016 and transformed the hospital in a phase-wise manner by December,” said Ayyaj. “The biggest issue was manpower. Just 12 nurses were managing the entire 100-bed hospital in a small area with enough space to accommodate just 30 beds.”
The district hospital lacked basic facilities — no surgeries happened here; there was no blood bank and the lab facilities were primitive. The staff included three specialists, a surgeon and a gynaecologist and 6-7 MBBS doctors.
The first step was to recruit the support staff. The number of nurses went up from 12 to 45 — those from Bijapur were given first preference, a few were hired from nearby districts like Dantewada, Kanker, Bastar and then from the rest of the state.
Desperate situation and an SOS
The next step was to hire doctors. But who would come to Bijapur? Ayyaj was getting desperate and frustrated. One night, he wrote a message and circulated it on WhatsApp and Facebook. The message read:
“I am Dr Ayyaj, a medical graduate who joined the Indian Administrative Service. Currently, working as district collector, Bijapur (Chhattisgarh). My district is predominantly tribal, densely forested and Naxal-affected. We are developing (a) district hospital … need post-graduate doctors and general duty doctors.”
Surprisingly, he received 46 resumes from specialists and 66 from MBBS doctors from states bordering Chhattisgarh and from the rest of the country. How the doctors were hired is an interesting story.

Some came, some were bartered for
“Dr Arun Chaudhury was the first guy who came. He had just got married. It was a love marriage, and he was thrown out of his family. I asked him to visit Bijapur. It was monsoon time, and Bastar was resplendent in all its beauty. The couple decided to stay back,” said Ayyaj.
“The second doctor I hired had earlier come to Bijapur in 2013, but didn’t stay back because of the remoteness of the area and the lack of infrastructure. This time I convinced him. I didn’t have any anaesthetist. I was visiting Basaguda, 39 km from Bijapur, and I came to know of a CRPF guy who was an anaesthetist, but was doing general MBBS duty there. I spoke to the DIG of CRPF and asked him to give this guy to me and, in lieu, I gave him one MBBS doctor. I then asked this CRPF guy to get his wife along, who was a pathologist. That’s how I got the blood bank running. There was a paediatrician working in Saudi Arabia, but wanted to move back to India. Many gap-year students also joined.”
The selection process was kept simple. A committee of three, comprising a civil surgeon, the chief medical and health officer (CMHO) and Ayyaj himself, was formed. The applicants could send their CVs on WhatsApp. The committee just cross-checked their registration number on the Medical Council of India website and conducted tele interviews.
“Under the National Health Mission, we asked a few heads of departments (HoDs) to be mobilised from medical colleges across India. We got HoDs from Aligarh Muslim University and Kakatiya University in Telangana. We got two people from Warangal and Khammam. We also got medical officers from Maharashtra. The reason the functionality of the hospital never came down was because those who left always gave us their replacements,” said Ayyaj.
Bumper salaries, great infrastructure
Those from outside were apprehensive about moving to Bijapur. The place was remote and there were security issues. Back then, there would be no mobile network for 2-3 days at a stretch.
“The first thing I did was to make a comfortable living setup for these doctors. I had two spare buildings meant for a course for auxiliary nurse midwives (ANM), which never took off. We converted their hostel building into our residential complex where we made 12 one bedroom-hall-kitchen setup which had all the facilities like washing machine, TV, fridge, sofa set, bed, common laundry area, etc. The doctors just had to move in with their bags. Their pickups were arranged from Raipur itself and I appointed a guy to arrange for their gas connection, SIM cards and bank accounts.”
To keep these doctors entertained and motivated, informal gatherings were arranged every 10-15 days; cricket matches and dinners were organised. But the biggest pull were the hefty salaries paid to these doctors. Ayyaj offered salaries either on a par or more than those offered in urban areas. These salaries were 2.5 times more than what the other places offered.
The logical question: How were the funds arranged for?
Funds were mobilised from three resources. The first was the District Mineral Fund (DMF) — it was the royalty received from the NMDC mines in Dantewada; Bijapur got some share, which then was Rs 42 crore per annum. The other source was the NMDC CSR through which Bijapur got Rs 14-15 crore. Funds were also received through a Special Central Allowance given to Naxal-affected areas. The entire corpus came to Rs 28 crore.
“We also got some funds from the National Health Mission. We submitted a plan and based on its approval; loan was granted. The loan we got through the DMF was later shifted to the NHM, so the recurring cost of manpower and equipment was taken care of by the NHM. The NHM also sanctioned a maternal child care hospital for Bijapur and we got an additional loan for a 50-bed child hospital,” said Ayyaj.
Giving them the respect that they deserve
“Investing in infrastructure is the key. As a district collector, when I sit in my AC chamber, my efficiency is more. We installed ACs in the doctors’ chambers. We transformed the chambers by putting good chairs, good curtains … they were satisfied. I also gave them one attendant each, whose job was to call patients and draw the curtains,” said Ayyaj.
He even gave them an additional Rs 15,000 each to decorate their areas. It gave them a sense of ownership. He arranged a gathering of nurses every six months, where they could perform; those who were doing good work were felicitated. Flexibility in taking leaves and choosing shifts as per their convenience was also encouraged.
“I took care of small things. For example, doctors no longer want to do medico-legal duties. We made a provision that only MBBS doctors would do post-mortems. We improved the condition of our mortuary; it is as good as an operation theatre now,” said Ayyaj.
Emphasising that healthcare is human resource-intensive and there is no substitute to providing better work conditions, Ayyaj said: “We have created certain positions — like a biomedical waste manager. There is no such post in any government hospital in the country. His only job is to ensure proper disposal of biomedical waste. Then there is a floor manager whose only job is to ensure doctors are available and to see if patients need something.”
If Bijapur can do it, why can’t other places?
In Naxal-affected areas, people usually don’t enter cemented buildings as the general perception is that Naxals target such buildings. Around 95% of healthcare centres are near police camps. When people enter these buildings, Naxals see them as informers.
“To deal with this problem, I started the ‘haat bazaar’ scheme. I made a lady sit in the bazaar with an umbrella once a week. Her face gradually became familiar and she could then visit the interior villages. The Naxals wouldn’t stop them either. This project is now a full-fledged government project called the Mukhyamantri Haat Bazaar Clinic Yojana,” he said.
The major problem in providing health care, according to him, is that doctors at primary health centres end up referring 90% cases to the district hospitals because of which crucial time is wasted in providing medical attention. It also causes inconvenience to those living in the interiors.
“So, while we focussed on the district hospital in Bijapur, we also strengthened the primary health centres and community health centres in Bijapur. However, we made sure that the patients automatically come to the district hospital. We even purchased bikes so that doctors could visit the interiors.”
Bijapur was a greenfield — there were no private hospitals then, there aren’t any now. “We strictly told those working in our district hospital to not undertake any private practice. My policy was very clear. I told them that this district is dependent on the public health system, so we shouldn’t be sending them to private hospitals. Besides, I was paying them salaries of Rs 1-1.5 lakh. Why should I encourage that (private practice)?” asked Ayyaj.

‘Put money in public institutions’
In 2018, the central government laid down guidelines for facilitating the entry of private sector in healthcare at the district level through the public-private partnership (PPP) model.
Asked if this model will work, Ayyaj said: “The problem is that we are still following the Bhore Committee recommendations of 1946, which gave us the institutional structure of PHCs, CHCs and district hospitals. However, then there were no good roads, no transportation facilities, and connectivity was a major problem. But now we have a good network of ambulances, so we shouldn’t focus on upgrading the PHCs. Instead, we should focus on making our district hospitals better. There is a reason why you will find poor people lying on the floor in government hospitals. One, they don’t have the money and second, no private hospital will entertain them. We should bring our district hospitals to such a level that the middle-class feels comfortable visiting these hospitals. The doctors will also like it if they will get a variety of patients and not just the poor who are not very particular about hygiene.”

