Rural India has just one question about the COVID-19 vaccine — “Will it be free for us?”
Rural India deals with harsh realities such as starvation and lack of access to healthcare. They have to be factored in too as India gears up for a gigantic COVID-19 vaccination programme.


While a pandemic-scarred world awaits a vaccine that can provide sufficient protection against the novel coronavirus disease (COVID-19), and scientists track each step in the development of each vaccine candidate in its final phase, in rural India ordinary people are asking only one question –— will it be free of cost?
Vaccine talk has started in Willkisan Nagar village in Odisha’s Khurdha district as in so many other villages across India. The village, originally called ‘nua gaan’ (new village), and re-named after W Wilkinson, a British magistrate in the early 19th century, has a population of over a thousand people and a health and wellness sub-centre.
“The people here are quite excited. They are waiting for the vaccine. They know that doctors, nurses, health workers and those in the frontline of the battle against this virus will get vaccinated first. It is all over the news. But, as I go round the villages, they ask me: ‘What about us? Will it be free for us?’ Then, they ask ‘If it is not free, how much will it cost?’” says auxiliary nurse and midwife Mamata Nayak over a crackling phone line.
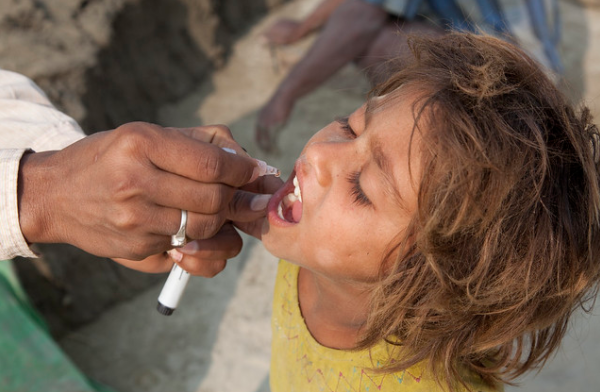
Nayak sends a photo of the Village Health Nutrition Day being observed at the Willkisan Nagar sub-centre, part of her routine duties that will continue even as preparations for the rollout of the COVID-19 vaccine gather momentum across the country.

It is tough to say which of the various COVID-19 vaccines will hit the market first. Vaccines can be made available to the public only after they go through regulatory processes; no one can put a date on which vaccine candidates would pass all the required criteria and when. Government spokespersons say a broad blueprint of the vaccine rollout is ready, and from “March to May” vaccines are likely to be available in significant numbers. They will be progressively rolled out over the years using the national immunisation programme.
Last week, Principal Scientific Adviser K Vijayraghavan said about 300 million people will be part of the first “wave” to get the COVID-19 vaccine in India. They consist of healthcare workers, police personnel, those above 50 and those younger with underlying illnesses that make them more vulnerable.
How will this gigantic exercise pan out in rural India, where the vast majority of India’s population still lives? While ordinary people worry if the vaccine will be made freely available to everyone, there are other issues related to how the COVID-19 story will unfold in villages and remote corners of the country.
Sulakshana Nandi, National Joint Convener of People’s Health Movement India, worries most about “how the COVID vaccination programme would impact other ongoing health programmes, including routine immunisation. Where is the budget to hire more trained health workers who will do social mobilisation in the run up to the vaccine rollout and carry out vaccinations”, she asked.
“It is not clear at all. We have seen what is happening already, with other diseases pushed to the background and health workers focussing only on COVID-19 related tasks. This will intensify with vaccine rollout and the entire energy and budgets of the health ministries will go into COVID-19 vaccination,” Nandi added.

If outsourced to the private sector, there are issues of cost, accountability and equity, as evidenced from previous experiences in outsourcing of health services. “Will a private agency go to the remote areas? Finally, it is about affordability. What happens once health workers get the vaccine? What criteria will be used to decide who gets the vaccine free?” asked Nandi.
Prabir Chatterjee, who works in the non-profit Amader Haspatal (Our Hospital) in Sarenga Phulberia, a tribal-dominated village in West Bengal’s Bankura district, feels somewhat the same way. The work of collecting the list of all health workers, with their name, age and identity details, has started, but there is no getting away from the enormity of the supply chain and logistical challenges ahead, he said.
“There will be questions from those who are left out, whatever criteria be used to decide who gets the vaccine first. In the context of rural India, there are other issues. Where will the vaccines be administered? For children, anganwadi centres and schools may be used. But this is going to involve adults. The elderly who are included in the priority list will have to be taken to vaccination centres that may not be near. Who will take them? Then, there are issues of the cold chain. Do we have enough storage capacity, vaccine boxes? If not, what happens to the other vaccines? How will they be stored? My biggest worry is the impact on other ongoing health and immunisation programmes,” said Chatterjee.
With the entire health workforce concentrating on COVID-19 vaccination, what will happen to social mobilisation and advocacy needed for routine immunisation and other programmes? “We have seen this before. We remember a measles outbreak being neglected in Rajmahal during the Pulse Polio campaign. There were diarrhoea deaths without treatment because the health worker had to go for Pulse Polio duty near Barharwa (in Jharkhand). The effect of the nationwide lockdown on institutional deliveries and TB treatment in April was very negative. Will there be quiet budget cuts for other health programmes because of this mass COVID-19 immunisation programme? If the task is done as a public-private partnership and the private sector comes in the vaccine rollout stage, what happens to the grand plans of strengthening health systems? Finally, there is the issue of biowaste. Have we started thinking about how we are going to dispose of this huge number of syringes etc without creating a health and environmental hazard?” Chatterjee asked.
Nearly four million doctors and nurses power India’s immunisation programme, but India will need more to carry out COVID vaccinations, as a recent BBC report observed. Does this mean that the road ahead is totally bleak? Not necessarily. Not if one recognises that there is a huge difference between vaccine and vaccination, and that vaccinating hundreds of millions of adults for the first time against COVID-19 is going to be a gigantic task, especially when it is happening at the time of an acute economic crisis and mounting malnutrition that reduces immunity.
India saw one of the most stringent lockdowns from April to May this year. This resulted in a massive crisis of stranded migrant workers, and a resultant food security/hunger crisis, pointed out Dipa Sinha, Assistant Professor (Economics), School of Liberal Studies, Ambedkar University. She was speaking at a webinar organised by the Peoples’ Health Movement as part of the Prince Mahidol Award Conference.
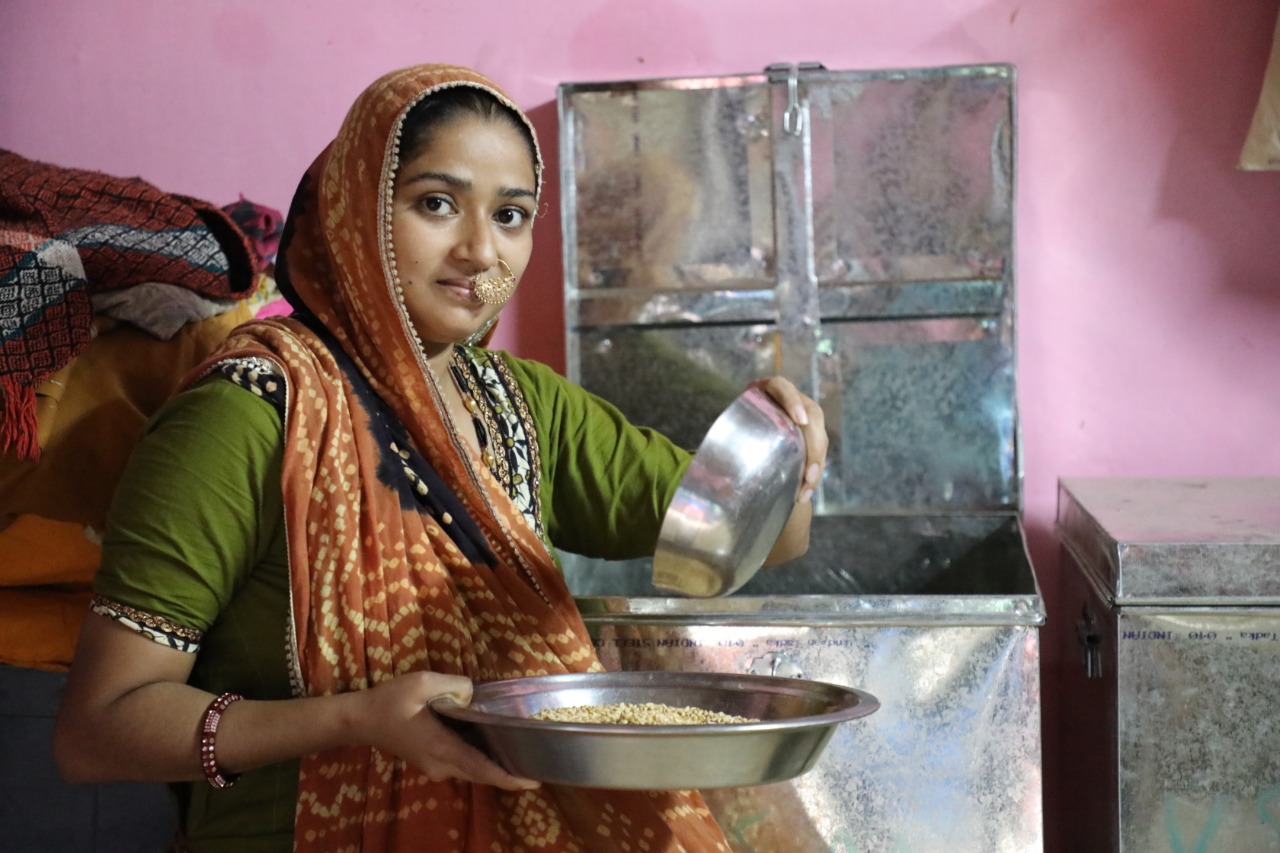
Sinha noted that phone surveys have shown very high levels of hunger, reports of starvation, and that over 200 deaths due to starvation and financial distress had been reported from March to July. Additionally, closure of schools and early childcare centres took away one important source of nutrition, especially for women and children, she pointed out.
The Right to Food campaign, of which Sinha is an active member, in partnership with several civil society organisations initiated ‘Hunger Watch’, a rapid survey across 11 states from mid-September to mid-October. The idea was to get a sense of the extent of hunger among vulnerable groups, as well as to take immediate local action to support those in extreme need.
At the Peoples’ Health Movement webinar, Sinha pointed out some of the findings of Hunger Watch – compared to the pre-lockdown months (February-March), the situation between September and October in sampled households showed 50 per cent less cereal consumption, 62 per cent less pulse consumption and 67 per cent less egg consumption, among other things.
This is very serious. But there is still time. Such harsh realities as well as ground reports about other health issues need to be factored in as India gears up for a gigantic COVID-19 vaccination programme.
Patralekha Chatterjee is an award-winning journalist/columnist, and photographer focussing on development issues. Currently, her writing focusses on the intersection of politics and public policy on a range of inter-linked development issues for Indian and international media.
(Views are personal)
Also Read: Safety, shortage and scaling-up: How prepared is India for the arrival of the COVID-19 vaccine?

