Blood shortage brought on by the lockdown continues; thalassemia patients in extreme distress
Every day 27 children with thalassemia are born in India. This genetic blood disorder requires regular blood transfusion for lifetime. Since the lockdown, blood banks are facing an acute blood shortage

Nine years back, when Kalanaika M, a resident of Maisooruammanadodi village in Anekal block of Bengaluru Urban district, became a father for the first time, his joy knew no bounds. All the 60-70 families in his village — a village of Banjara (nomad) community — celebrated his son’s birth.
Kalanaika named his son Jeevan, meaning life in English. But, the baby kept falling sick.
“I have studied till class 5 only and didn’t understand what was happening to my son. I took him to various temples and showed to local doctors. But, no improvement in Jeevan’s health,” Kalanaika told Gaon Connection. Then he took his son to a hospital in Bengaluru where he was told Jeevan has thalassemia, a life-long blood disorder requiring regular blood transfusion.
“By that time, my wife was already seven months pregnant with our second child, so we could not abort. My second son, Madan, also has thalassemia major,” he said.

In the last nine years, Kalanaika has sold off his cows and goats, leased out the only small patch of his farmland, and moved closer to Bengaluru, the state capital of Karnataka, to ensure his sons receive blood transfusion every three weeks. He works in a candle-making factory and earns Rs 10,000 a month. His monthly house rent is Rs 4,000 alone. But, he has never faced the trauma he has been living through in the last almost three months of the coronavirus disease (COVID-19) lockdown.
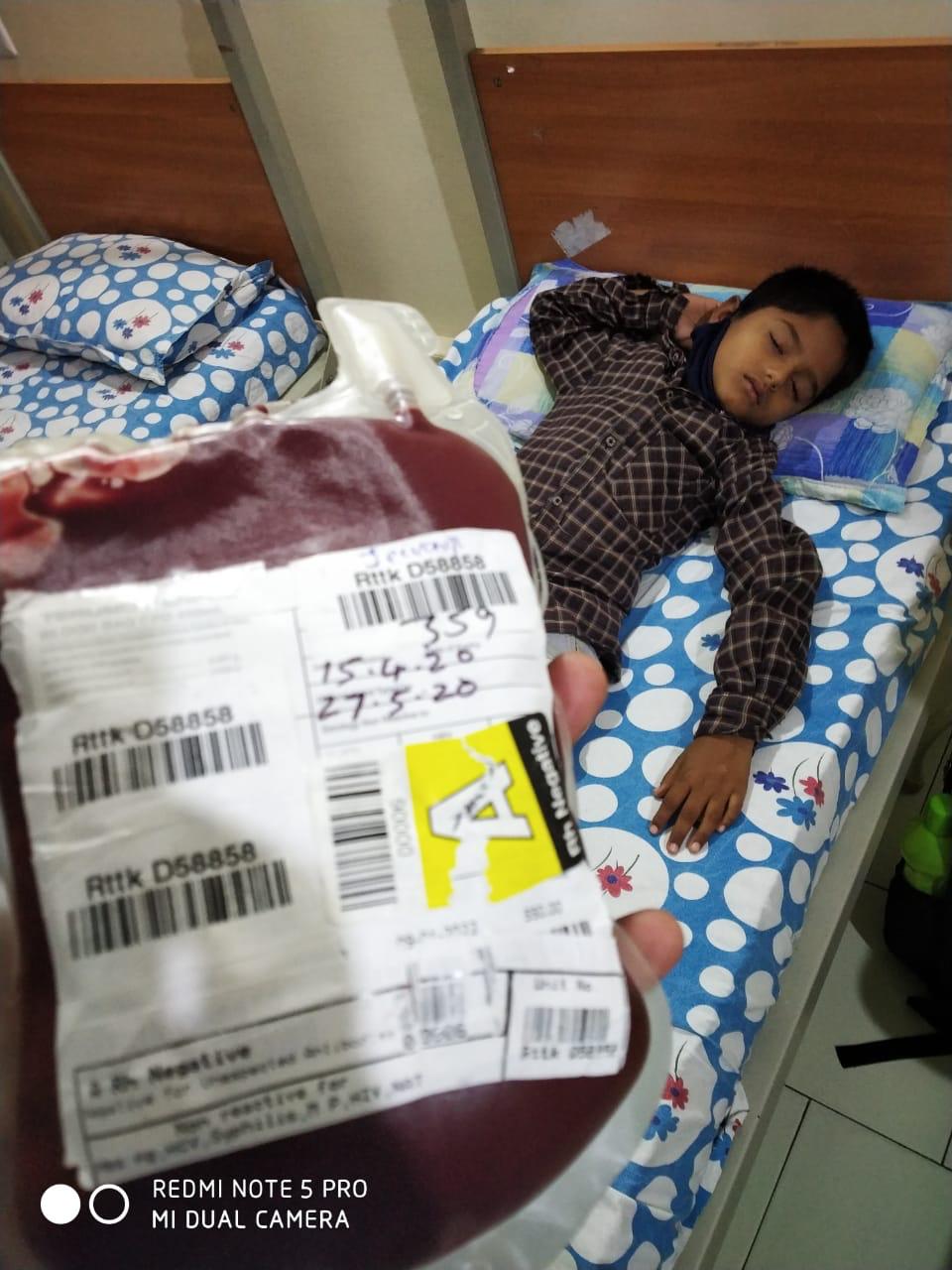
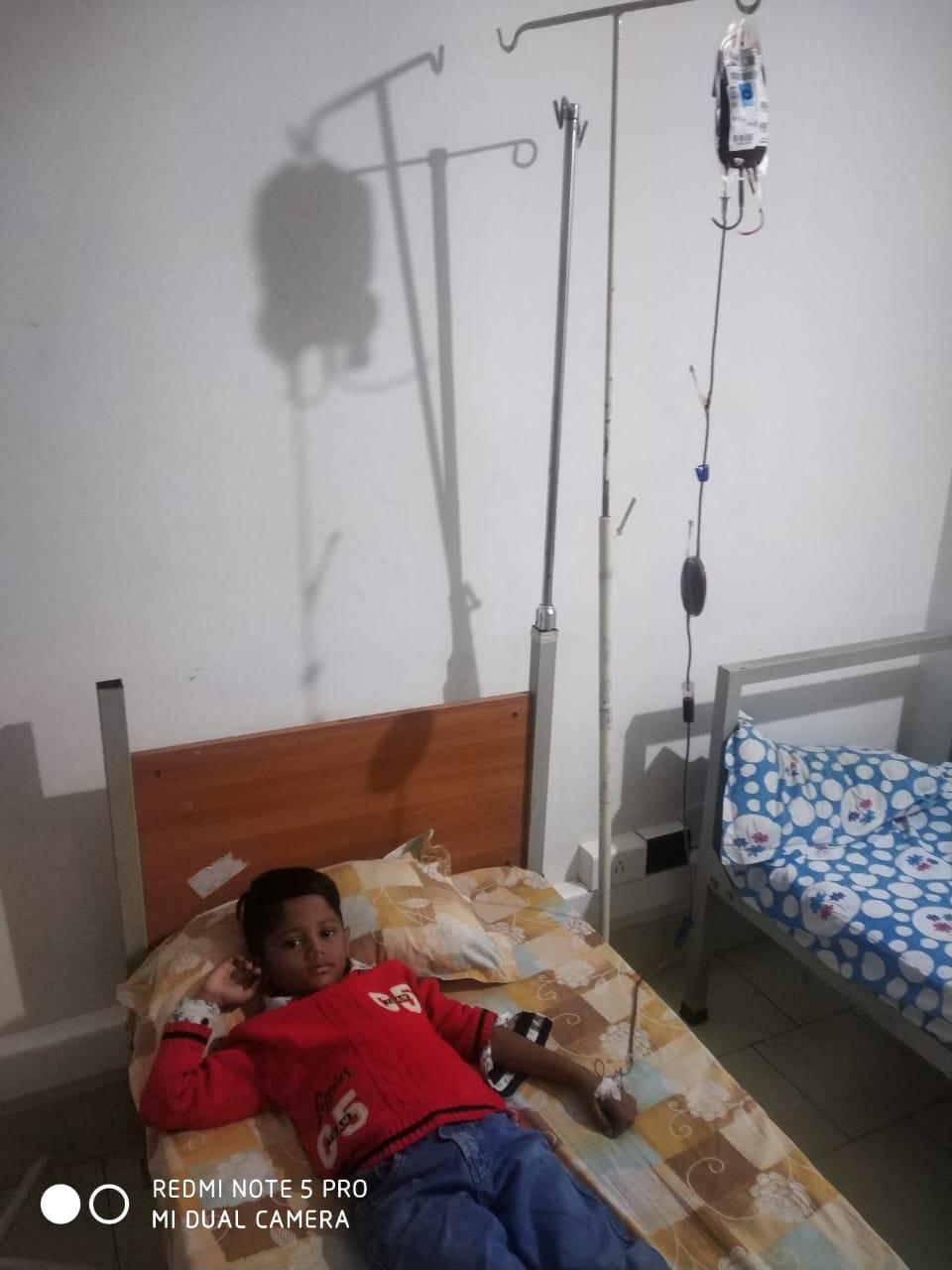
“Both my kids need 300ml blood each for transfusion. Blood banks do not have blood and people are not coming forward to donate blood because of the coronavirus. I cannot sleep in the night thinking how I will organise the next blood transfusion for my sons, which is just a couple of days away,” said a worried Kalanaika.
Because of the COVID-19 lockdown, there is an acute shortage of blood in blood banks across the country and several thalassemia patients, who need regular blood transfusion, or else it can be fatal, are running from pillar to post to organise blood units. And it isn’t the thalassemia patients alone who are suffering due to the blood shortage in the country. Cancer patients, pregnant women, accident victims, emergency patients, etc are all under extreme stress.
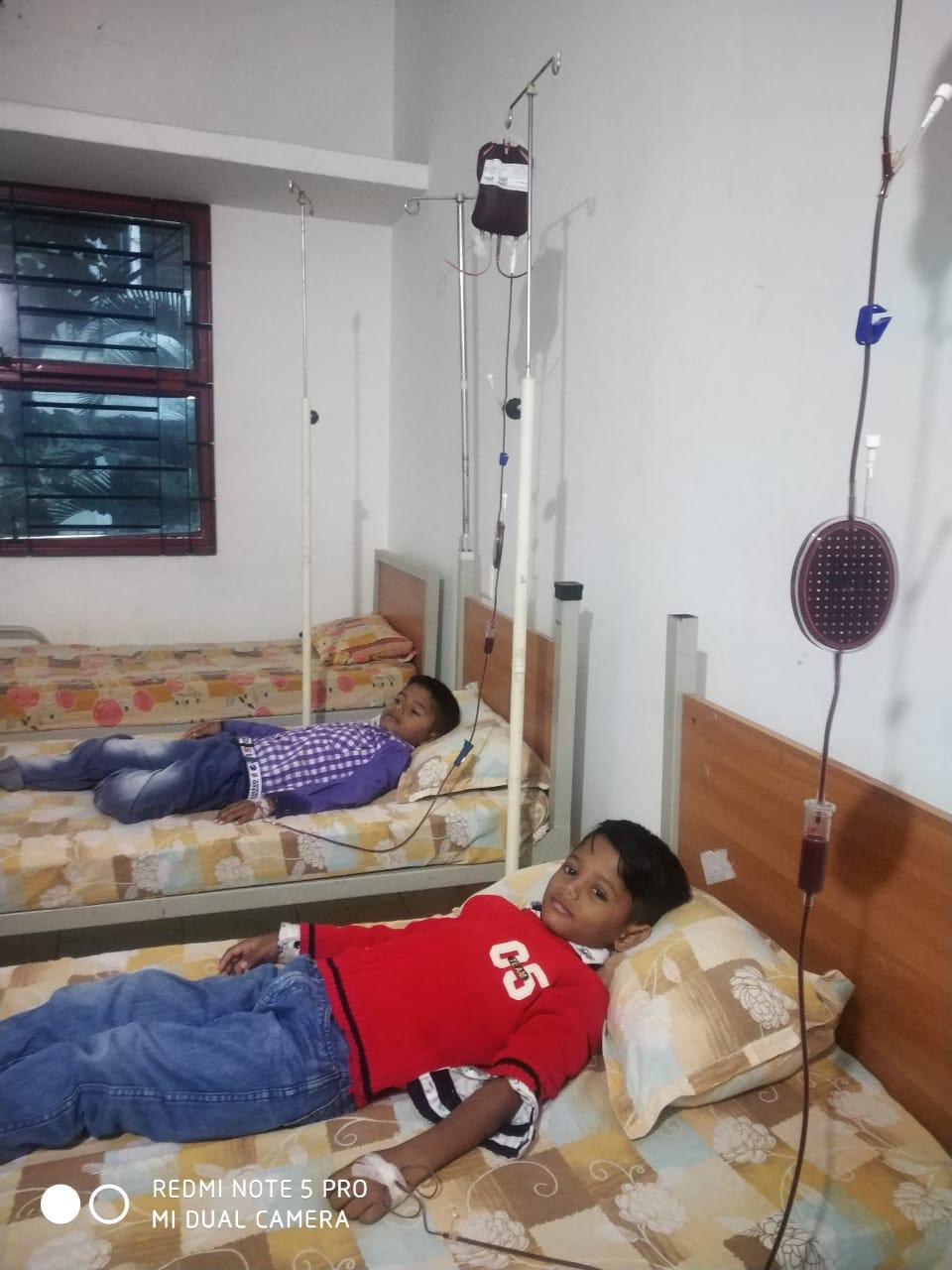
“We used to collect about 4,000 units of blood a month from the voluntary blood donors. This was used for thalassemia patients who need blood all their life, pregnant women, accident cases, cancer patients and many other patients,” Latha Jagannathan, medical director and managing trustee of Rotary-TTK Blood Bank, Bengaluru, told Gaon Connection. “Then COVID-19 happened and our blood collection has gone down to 1,000 units a month. But, patients still need blood. I want to appeal to the voluntary blood donors to come forward and donate blood and save lives,” she added.
Burden of thalassemia in India
Thalassemia is a genetic blood disorder in which a patient cannot make enough red blood cells (RBC) and needs to be supplemented with RBC transfusions every two to three weeks to stay healthy and to survive. There are different types of thalassemia — alpha thalassemia, minor/carrier/trait thalassemia, thalassemia intermedia, and thalassemia major.
Kalanaika’s both the sons have thalassemia major in which the red blood cells are destroyed almost as soon as they are produced and the bone marrow cannot produce a sufficient number to replace them. This condition requires intensive medical care.
Thalassemia is an inherited disorder and is passed from parents to children through genes. People who inherit the defective haemoglobin genes from one parent, but normal genes from the other are called carriers. Carriers often have no signs of illness other than mild anaemia, but carry the defective gene.
India has a huge burden of thalassemia, which is a major public health concern. Every year 10,000 children are born in the country with thalassemia, which accounts for about 10 per cent of the total world incidence of thalassemia-affected children, informs a 2019 paper, ‘Need for a universal thalassemia screening programme in India? A public health perspective’, published in Journal of Family Medicine and Primary Care. Also, one in eight thalassemia carriers live in India and there are nearly 42 million carriers of the β-thalassemia trait in the country.
“I am 42 years old now and a thalassemia intermedia patient. I have been on blood transfusion since I was diagnosed with this disorder at an age of five years,” Namitha A Kumar, head of advocacy with Bengaluru-based Open Platform for Orphan Diseases, told Gaon Connection. She is also a scientific writer with Strand Life Sciences Pvt Ltd, Bengaluru.
“Never before did I ever face a situation where the blood bank informed it did not have blood. And, we cannot blame the blood banks, as blood donation camps are not being held and blood donors not coming forward due to the fear of coronavirus,” she added.
Kumar and others are reaching out to the resident welfare associations in the city to organise blood donation camps by following physical distancing measures and taking all the necessary precautions. “Last week, we organised a blood donation camp in a 200-apartment gated colony in Bengaluru where 21 voluntary blood donors came forward. We need more such campaigns,” said Kumar.
Blood banks, such as the one run by the Rotary-TTK Blood Bank, are a lifeline of thalassemia patients as they provide free blood to the patients. “Initially, I used to get blood units and transfusion through a private facility. For each of my child, one month cost used to come to Rs 4,000-5,000,” informed Kalanaika.
“For the last four years now, I am getting blood [free] through TTK Blood Bank. The Karnataka government also provides subsidised medicines to thalassemia patients. But, the lockdown has created hell for us. My family members have already donated blood. Whom do I approach now?” he asked.
Risk of COVID-19
According to Satendra Singh, associate professor of physiology, University College of Medical Sciences & GTB Hospital, Delhi, “The Rights of Persons with Disabilities Act, 2016 includes three hematological disabilities [thalassemia, hemophilia, sickle cell disease], which are also high-risk COVID-19 conditions.”
For instance, people with sickle cell disease often have underlying cardiopulmonary co-morbidities. These individuals are predisposed to pneumonia, pulmonary vaso-occlusive disease and an acute chest syndrome. “New research suggests that COVID-19 triggers vaso-occlusive crisis (sickle cell crisis). Saudi Arabia’s Health Ministry in April issued the ‘COVID-19 in Sickle Cell Disease Rapid Response Guidelines’, but no concrete steps in India,” said Singh.
Some patients with hemophilia may develop inhibitors and doctors in such situation prescribe immunosuppressants that suppress the immune systems and make patients more susceptible to COVID-19, he added.
In such a scenario, the decision to convert tertiary care hospitals into COVID-19 only hospitals has its own repercussions. “For instance, on June 2, the GTB Hospital was designated as COVID-19 only hospital. Hence, its hematological and thalassemia services have been suspended. All patients belonging to former category shall be referred to Chacha Nehru Bal Chikitsalaya Hospital, a children’s hospital. So, where will adults with thalassemia go?” he questioned.
Keeping in mind the possibility of blood shortage due to the lockdown, on March 25, the National Blood Transfusion Council under the Union ministry of health and family welfare, issued the ‘National Guidance to Blood Transfusion Services in India in light of COVID-19 Pandemic’.
This advisory recommended “in-house blood donation as well as outdoor blood donation activities may be continued, while ensuring compliance with extant social distancing norms, infection control guidelines and biomedical waste disposal rules.” However, there continues an acute shortage of blood in the country.
Meanwhile, India has a screening programme (Rashtriya Bal Swasthya Karyakram) for early detection of thalassemia and intervention for the children. But, the public health experts are demanding a universal screening programme in the country.
No doubt, the COVID-19 pandemic has brought the world on its knees. But, even in this health crisis, donating blood can save lives.

