COVID hits tribal districts: In April 2021 alone, Gadchiroli reported as many cases as it did between March 2020-2021
Between March 2020 and March 2021, Gadchiroli had about 10,000 documented COVID cases and 100 deaths due to the virus. But, in just April 2021, the tribal district has reported approximately the same number of cases and deaths.


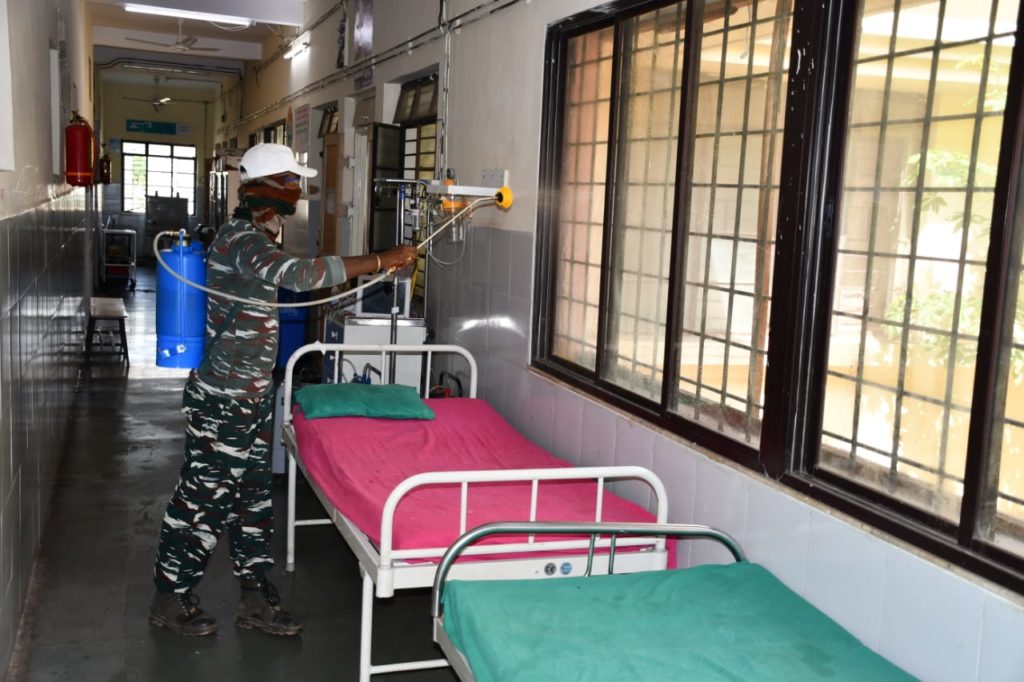
Sanitisation of Rural Hospital Wadsa in Gadchiroli, Maharashtra. Pic: Twitter/@192bncrpf
About nine per cent of India’s 1.38 billion population consists of tribal people. They belong to Adivasi communities who have always been pushed to the fringes, and rarely make it to the media spotlight unless the visit of a senior minister or an international diplomat demands a tribal dance, a mandatory peek into tribal culture.
Predictably, little is known of how the COVID19 pandemic is affecting the country’s tribal regions, which are mostly located in forested or hilly terrains without proper infrastructure or, sometimes, even a motorable road. The nearest PHC (primary health centre) could be several kilometres away.
Gadchiroli in Eastern Maharashtra, with over a million population, is a tribal district. And, if COVID situation in this district is anything to go by, the virus has penetrated deep into tribal regions in the second wave, and many Adivasis are dying.
Also Read: A tweet opens a Pandora’s box of how rural India is coping with the COVID19 second wave
“Between March 2020 and March 2021, Gadchiroli had about 10,000 documented COVID cases. But, in the last one month alone, in April 2021, the tribal district has reported approximately the same number of cases,” Yogesh Kalkonde, a physician and public health researcher, told Gaon Connection. Kalkonde works at the SEARCH (Society for Education, Action and Research in Community Health), an NGO working in Gadchiroli. He is also a practising doctor at the rural hospital of SEARCH, which works with the tribal communities.

“What is more worrisome is that the virus has reached tribal areas and the intensity in the second wave is very high,” Kalkonde said.
Official data and the one compiled from local news reports shows that between March last year and this year, about 100 deaths due to the virus were reported in Gadchiroli. However, in the last one month alone, in April 2021, COVID has killed 100 people in the district, setting the alarm bells ringing.
Just a couple of days ago, there were news reports from Odisha where members of particularly vulnerable tribal groups (PVTGs) tested positive. As many as 21 tribal people across eight different PVTGs, including two from the secluded Bonda tribe known for its secluded lifestyle, in the state have so far tested positive, The Hindu reported on May 14. Apart from the Bonda, members of the Dongria Kondh, Kutia Kondha Didiya, and Saura tribes have also tested positive. It is being speculated that the tribal people picked up the virus from the weekly haats.
Also Read: ASHAs brave the second wave of COVID19. Without masks, sanitisers and rightful remuneration
Last month, there were reports of how a number of COVID patients from the predominantly tribal districts of Gujarat were arriving at the New Civil Hospital in Surat. Most of them came from Bharuch, Narmada, Tapi and Dang districts.
The situation was not this dire in tribal areas last year in the first wave. A survey conducted last September by the Indian Institute of Technology Delhi, for the Ministry for Tribal Affairs, had found there was no major outbreak of Corona in 117 districts, with 25 per cent or more tribal population. It found about three per cent of the tribal population infected by the virus.
But, in the second wave, the virus seems to have hit tribal belts in a big way, and Gadchiroli, with 100 COVID deaths in a month, is only a snapshot of it. This is a matter of great concern as these Adivasi regions lack even the most basic health facilities. And taking the message of COVID 19, its precautions and vaccination poses a big challenge in these remote locations.
“What we are seeing in villages is fear. Much like other villagers, tribal people do not want to get tested for Corona or be hospitalised,” said Kalkonde. “And while we take the message of COVID testing and vaccination to tribal areas, we must not lose sight of the fact that the tribal population has its own social behaviour based on various sociocultural factors, which is not well understood or respected by the government or the urban population,” he added.
For instance, tribal communities have their own strong social customs around death. Dying alone in a hospital with no final closure can be unnerving to them, which is why the hesitancy to get tested for COVID-19, or its vaccination.
“It took decades to get the message across for immunising kids in these tribal communities. They trust ‘lived experiences’ more than what is written in the books,” said Kalkonde.

As the virus spreads to tribal areas, the response has to be at two levels — short-term and long-term — claim public health experts. Behavioural change is a long-term process and may take years or decades, but some quick short-term measures need to be taken to minimise loss of lives.
“In the short term, we need to focus on using technology to try and save lives by delivering medical equipment oximeters to health centres in tribal areas and creating oxygen facilities within a radius of 50 kilometres or so. Low tech solutions like oxygen concentrators are the need of the hour,” said Kalkonde.
Apart from this, through local tribal leaders (Adivasi communities listen more to their leaders than government officials or doctors from outside), there is a need to inform the tribal population about the danger signals of COVID19 so that if anyone faces breathing difficulty, rising fever or general weakness, the person should immediately be brought to the nearest health centre. Medical staff at primary health centres need to be quickly trained in operating oxygen concentrators, and in using non-invasive ventilators at district hospitals.
Also Read: With no tests and no treatment, people in rural India are dying of COVID-like symptoms

