Profit at the cost of the poor: NITI Aayog’s proposal for public-private partnerships in healthcare
Implementing the Central government’s proposal to privatise district hospitals could be disastrous for India’s poor. The government should learn from successful initiatives in some of the most conflict-affected districts that have strengthened their district hospitals.


Photo: LocalBizNetwork2012/flickr
Sulakshana Nandi and Deepika Joshi
One year into the NITI Aayog’s proposal to hand over district hospitals to private medical colleges, many states seem to be going ahead with it, despite previous failures of public-private partnerships (PPP) in healthcare. In May 2020, in the midst of the pandemic, the NITI Aayog had sent reminders to states to speed up implementation of this proposal.
A review of media articles shows states are at different levels of planning and implementing this proposal. One aspect about this proposal is that the NITI Aayog is trying to push this scheme on a priority basis in Aspirational Districts. However, in many states there is active opposition to such partnerships from various quarters. Aspirational Districts are those districts affected by poor socio-economic indicators. These are aspirational in the context that improvement in these districts can lead to overall improvement in human development in India.
The Uttar Pradesh government is planning to open one medical college in all 75 district under this public-private arrangement, with the state chief minister Yogi Adityanath calling it an “opportunity for investors”. In December last year, West Bengal invited an ‘expression of interest’ from private medical colleges to use public hospitals.
Also Read: How did India’s most populous state Uttar Pradesh lead the COVID-19 battle?
The Union Territory of Chandigarh’s health department has proposed establishing a medical college in the existing Government Multi Specialty Hospital in Sector 16 in partnership mode. This was immediately opposed by health workers’ unions in the hospital.
The Madhya Pradesh government’s move to privatise the Sanwer PHC (primary health centre) has been opposed heavily by health groups. In Nagaland, the proposed construction of a medical college through partnership has run into trouble from the local people over the private hospital land, days after the foundation stone was laid by the Union health minister.
Meanwhile, in Goa, the South Goa Hospital partnership has been vehemently opposed by opposition parties. It is reported that the Odisha, Maharashtra and Karnataka governments are mulling implementing the NITI Aayog’s proposal.
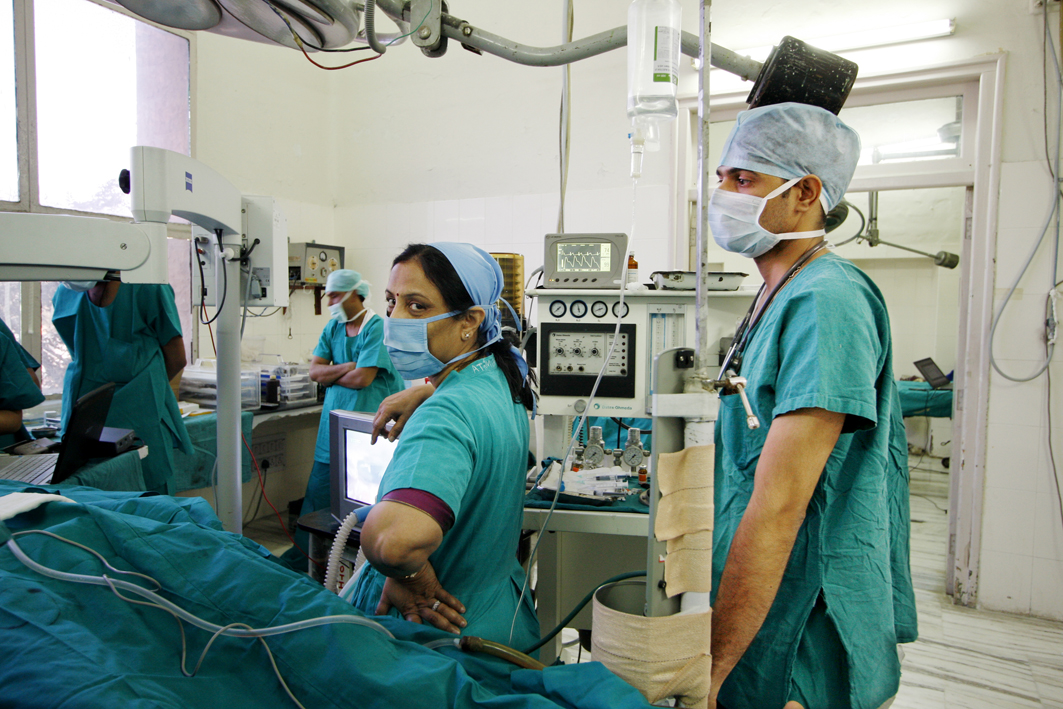
What is the proposal?
In January 2020, NITI Aayog had brought out a proposal for privatising district hospitals and linking them to new or existing private medical colleges through a ‘public private partnership’. They called for comments on the model contract and a stakeholder consultation. However, even before the consultations could take place, the finance minister announced this measure as part of the 2020-21 budget.
This proposal to privatise district hospitals is being done in the name of medical education. A reading of the draft model contract reveals that the proposal aims to convert government-run district hospitals into profit-making enterprises. It poses the danger of pushing thousands of families into poverty due to the increase in cost of treatment. It also goes against India’s National Health Policy 2017 and its global commitment to Universal Health Coverage.
There has been a lot of outrage against NITI Aayog’s and the government of India’s proposal from doctors, health administrators, health experts, academics and health networks such as the Jan Swasthya Abhiyan. Three state governments — Kerala, Chhattisgarh and Madhya Pradesh (then governed by the Indian National Congress; now by the Bharatiya Janata Party, which is in power in the Centre) had even rejected the proposal.

Why the uproar?
The contract proposes to hand over district hospitals for 60 years to private agencies that own or build private medical colleges. The private agencies will pay an extremely low fee for it and the government will provide additional grant, in the form of equity support, with possibility of giving land at a concession and viability gap funding.
The private agencies would have to raise other funds through bank loans or private financing methods. Therefore, they will need to keep making money to repay loans or pay their investors. This will have a disastrous impact on patients coming to hospitals for treatment from all over the district.
Ironically, right in the midst of the COVID-19 pandemic in May last year, the Centre introduced viability gap funding for the social sector, and asked states to speed up the adoption of this proposal with this funding. “The viability gap funding provided for economic infrastructure will now be extended to social infrastructure,” Union finance minister Nirmala Sitharaman said.

Increased cost of treatment
The most direct and catastrophic impact this model will have on patients is increased cost of treatment. The draft contract allows privatised district hospitals to have a category of ‘free patients’ (whose cost will be paid by government to private agencies), with the rest having to pay charges based on ‘market- competitive rates’. The proportion of ‘free’ out- patients has not been mentioned and the provisions around charges for the out-patient department are confusing. To be considered a ‘free’ patient, they would have to be certified by a district health authority, which, we know from experience, can be very difficult.
Currently, most patients coming to the district hospital are referred from lower government facilities such as primary health centres and community health centres for higher level treatment. Just imagine — a woman, referred from her block community health centre for emergency care, has to travel more than 100 kilometres from her village to get herself certified from the district authority to get this treatment for free. Else, she pays ‘market competitive’ charges.
The draft contract also allows for commercial enterprises to be set up for facilities such as food and accommodation. There seems to be no restrictions on charges to be taken from patients for these facilities that form crucial support systems for those who usually come from far-off and rural areas.
Allowing the district hospital to charge user fees for all services is against all previous announcements by the government on providing free healthcare. This will lead to an increase in out-of-pocket expenditure and catastrophic health expenditure for patients. This, when, already it is the main cause of people being pushed into poverty. All over the world, hospital user fees have been denounced as very problematic.
There is a provision for ‘regulated beds’ and ‘market beds’. ‘Regulated beds’ would most probably be used for patients enrolled in government health insurance schemes such as the Pradhan Mantri Jan Arogya Yojana and, therefore, paid by the government. However, as evidence shows, even when using the publicly-funded health insurance scheme in private hospitals, most patients continue to spend out of their pockets.

Over to private agencies
The draft contract also allows the government to hand over staff to private agencies. There is also the option of deputing staff, in which case, the government will continue paying their salaries. Staff can also resign from the government job and join the private hospital/college. It has been seen that most private medical colleges are unable to organise faculty as per Medical Council of India norms and, therefore, this provision is extremely advantageous for the private college/hospital. But, it will be a huge loss for the government and for the districts to hand over government specialists, doctors, nurses and other staff to the private sector.
Learning from successful initiatives
Instead of proposing to privatise district hospitals, the government should learn from successful initiatives in some of the most conflict-affected districts that have strengthened the district hospitals concerned. For instance, an initiative that started in the district hospital in Bijapur in Chhattisgarh, has now been replicated by the neighbouring Dantewada and Sukma districts.
Also Read: Meet the man who made the Bijapur District Hospital in Chhattisgarh one of the best
The district hospitals have been up-graded and services increased through recruiting and retaining doctors and specialists through innovative methods, and filling other staff, equipment and infrastructure gaps. Such attempts are also being made in other states such as Odisha.
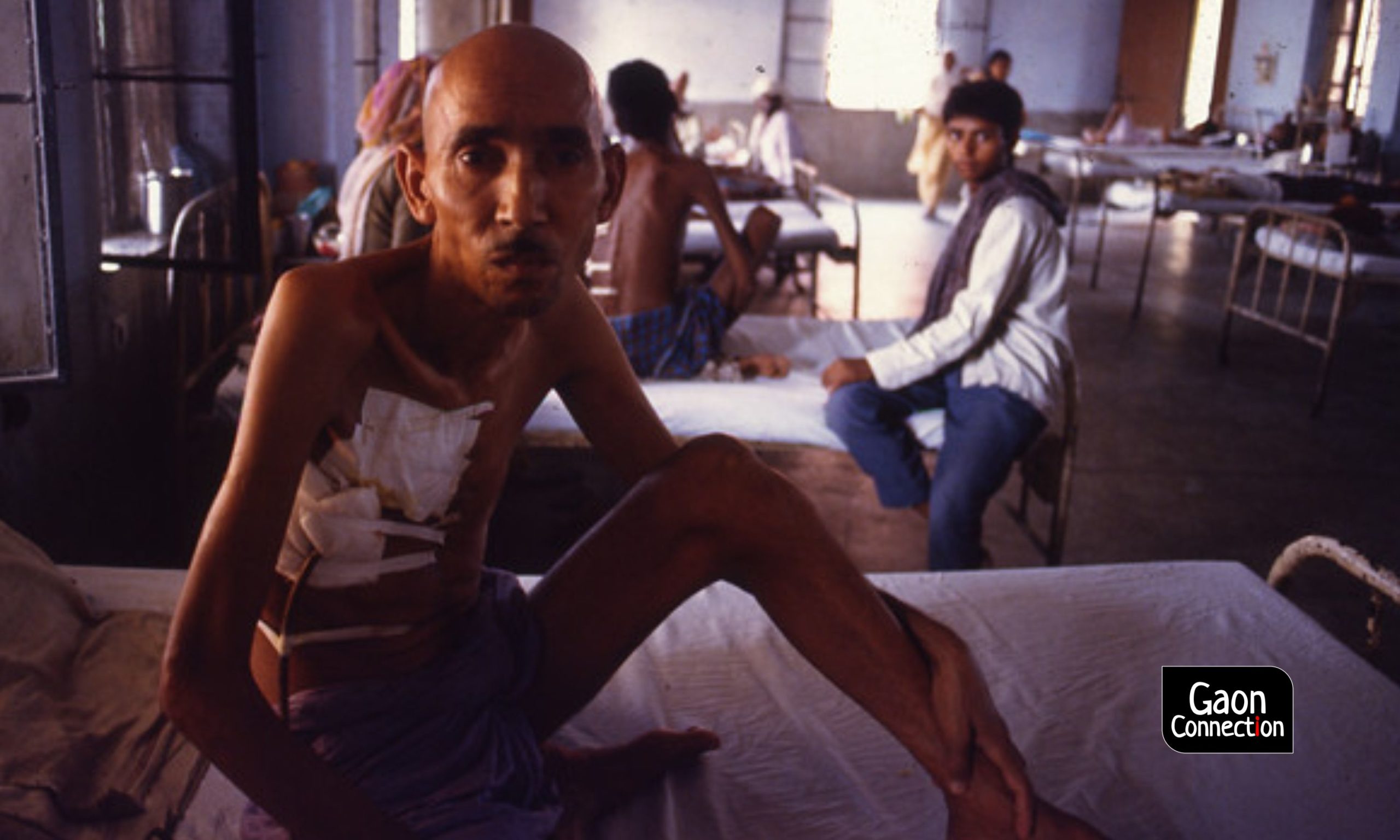
In proposing this public private partnership, NITI Aayog and the government of India clearly reject the idea of a government health services delivery system motivated by social logic and public good, and alter it with a revenue-generating enterprise model working on the profit motive.
The states going ahead with the adoption of the proposal too fail to understand these concerns. The disastrous implications of this proposal will first be felt by the most vulnerable groups — the poor, women, and adivasi, dalit and rural communities. At the global level, India may fail miserably on achieving the sustainable development goals, of which health expenditure by people is an indicator, if this proposal is allowed to continue. The government and the states need to abandon this disastrous and anti-poor move.
Sulakshana Nandi is national co-convener of Jan Swasthya Abhiyan (People’s Health Movement, India) and Deepika Joshi is a public health researcher associated with it.
Views are personal.

